Hormonal Belly Fat Causes and Solutions

If you’ve been eating well, exercising regularly, and still can’t seem to shake that stubborn midsection weight, you are not alone. Millions of American women face this exact frustration every day. The truth is, belly fat isn’t always about calories in and calories out. For many women, the real culprit is far more complex — it’s hormonal. Understanding the root causes and solutions behind hormonal belly fat is the first step toward reclaiming your body, Your confidence, and your long-time period health.
This guide is written for women across the United States who are tired of being told to simply “eat less and move more.” We’re going to move deeper. We’re going to talk about the real science behind hormonal belly fat, explain what’s happening inside your body, and — most importantly — give you actionable, evidence-based strategies you can start applying today.
What Causes Belly Fat in Females: The Hormonal Connection
When most people think about belly fat, they picture poor dietary choices or a sedentary lifestyle. But for women, understanding what causes belly fat in females requires a much closer look at the endocrine system — the network of glands and hormones that regulate nearly every function in the body.
Hormones act like chemical messengers. When they’re in balance, your metabolism hums along smoothly, your energy is steady, and your body maintains a healthy weight. But when even one hormone falls out of its optimal range, the effects can ripple through your entire system — and one of the most visible places that shows up is your midsection.
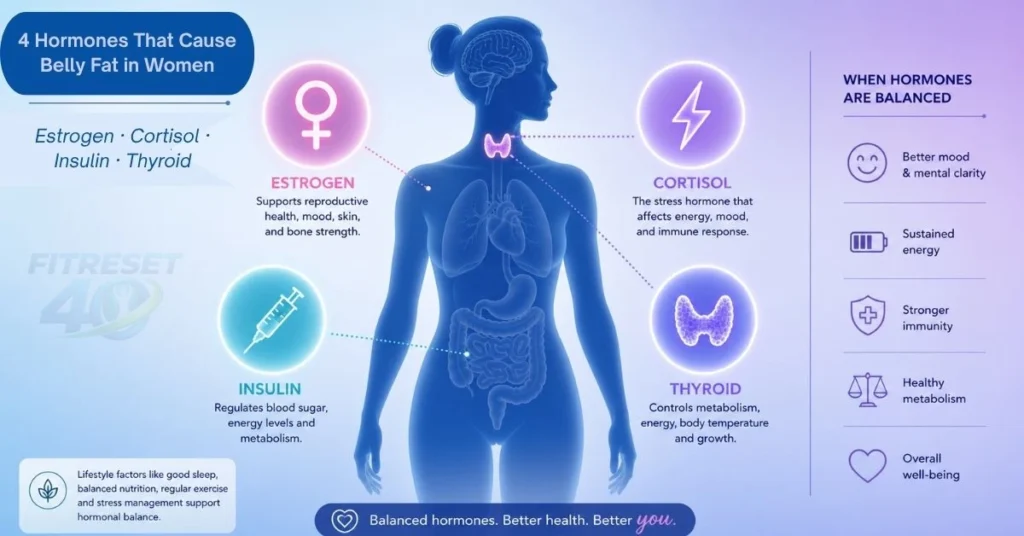
Here are the primary hormones that play a direct role in abdominal fat storage for women:
Estrogen: The Double-Edged Hormone
Estrogen is the primary female sex hormone, and it has a direct influence on where your body stores fat. When estrogen levels are high and balanced, women tend to store fat in the hips and thighs — the classic “pear-shaped” distribution. But when estrogen fluctuates — especially during perimenopause, menopause, or conditions like polycystic ovary syndrome (PCOS) — the body begins to shift fat storage to the abdomen.
estrogen decline and belly fat redistribution
Low estrogen, in particular, causes a redistribution of body fat from the periphery to the belly. This is one of the most common hormonal belly causes that many women entering midlife experience without even realizing what’s happening. They notice their jeans fitting differently, not because they’ve gained significant weight overall, but because the fat is moving.
Cortisol: The Stress Hormone That Builds Belly Fat
cortisol and abdominal fat storage
Cortisol, your body’s primary stress hormone, is another major factor in what causes belly fat in females. When you experience chronic stress — whether that’s work pressure, relationship struggles, financial worry, or even over-exercising — Your adrenal glands pump out cortisol continuously.
In brief bursts, cortisol is beneficial. It enables you to reply to danger. But chronically elevated cortisol tells your body to store fat in the abdomen, because abdominal fat cells have greater cortisol receptors than fat cells elsewhere. Your body essentially treats the belly as the safest energy depot during times of perceived threat.
Elevated cortisol also spikes blood sugar, promotes insulin resistance, increases appetite for calorie-dense foods, and disrupts sleep — creating a vicious cycle that keeps belly fat firmly in place.
Insulin Resistance: When Cells Stop Listening
Insulin is the hormone answerable for transferring glucose out of your bloodstream into your cells for energy. When cells become resistant to insulin’s signal, the pancreas compensates by pumping out more insulin. This chronically elevated insulin level is one of the most powerful drivers of abdominal fat accumulation.
insulin resistance and abdominal obesity
Insulin resistance would not show up overnight. It tends to develop gradually, often linked to a diet high in refined carbohydrates and sugars, lack of physical activity, terrible sleep, and continual stress. All of these factors are deeply tied to hormonal belly causes, making insulin resistance both a symptom and a contributor to the larger hormonal picture.
Thyroid Hormones: The Metabolism Regulators
An underactive thyroid, or hypothyroidism, is another important answer to what causes belly fat in females. The thyroid gland regulates your metabolic rate. When it’s not producing enough thyroid hormone, your metabolism slows down considerably — meaning you burn fewer calories at rest, feel fatigued, and are more likely to gain weight, particularly in the abdominal area.
hypothyroidism and unexplained weight gain
Millions of American women have undiagnosed or undertreated hypothyroidism. If you’ve been struggling with unexplained weight gain, fatigue, cold sensitivity, and difficulty losing belly fat despite your best efforts, it’s worth asking your doctor for a comprehensive thyroid panel.
Hormonal Belly Causes You Might Be Overlooking

Beyond the heavy hitters like estrogen and cortisol, there are several other important hormonal belly causes that women often miss — or that their healthcare providers fail to connect to abdominal weight gain.
Leptin Resistance: When Your Brain Can’t Hear “I’m Full”
Leptin is referred to as the satiety hormone. It signals to your brain that you have enough fat stored and that you should stop eating. But in many women — especially those who have yo-yo dieted or who are dealing with obesity — the brain stops responding to leptin’s signal effectively. This is referred to as leptin resistance.
leptin resistance and obesity research
When leptin resistance develops, the brain thinks the body is starving, even when it isn’t. It responds by increasing hunger, slowing metabolism, and encouraging more fat storage — especially around the belly. Leptin resistance is one of the more insidious hormonal belly causes because it creates a feedback loop that makes conventional dieting extremely difficult.
Progesterone: The Overlooked Hormone
Most conversations about female hormones center on estrogen, but progesterone plays an equally important role in body composition. Progesterone is produced primarily after ovulation, and its levels naturally decline with age and during menopause.
Low progesterone relative to estrogen — a condition sometimes called estrogen dominance — can cause water retention, bloating, And an boom in stomach fat. Many women who are told their estrogen levels are normal are never tested for progesterone, leaving this imbalance unidentified and untreated.
Sleep Deprivation and Ghrelin Spikes
Sleep is not a luxury — it’s a hormonal event. When you sleep fewer than seven hours in line with night, your frame produces extra ghrelin (the starvation hormone) and much less leptin (the satiety hormone). The result is that you wake up hungrier, less satisfied by food, and more likely to reach for high-calorie comfort foods.
Poor sleep also elevates cortisol, further compounding several of the hormonal belly causes we’ve already discussed. Over time, chronic sleep deprivation rewires your body’s hunger and fat-storage signals in ways that make belly fat far more stubborn.
Perimenopause, Menopause, and the Belly Shift
Perimenopause — the transitional period leading up to menopause that can begin in a woman’s late 30s or early 40s — is one of the most significant life stages tied to hormonal belly causes. As estrogen and progesterone fluctuate erratically before eventually declining, many women notice rapid changes in body composition, particularly in the abdominal region.
total 7 Natural Ways to Manage Menopause Symptoms
By the time full menopause arrives, the hormonal shift is complete, and fat distribution changes significantly. Postmenopausal women are far more likely to carry fat in the belly than premenopausal women of the same weight. This is not a failure of willpower — it is physiology. Understanding this is essential when asking what causes belly fat in females at different life stages.
Types of Belly Fat Female Bodies Store

Not all belly fat is the same, and knowing the different types of belly fat female bodies accumulate can help you identify what you’re dealing with and take targeted action.
Visceral Fat: The Hidden Danger
Visceral fat is the most dangerous of the types of belly fat female bodies store. It sits deep within the abdominal cavity, wrapping around vital organs like the liver, pancreas, and intestines. Unlike the fat you can pinch on your waistline, visceral fat is metabolically active — meaning it releases inflammatory chemicals and hormones that disrupt your metabolic function.
High levels of visceral fat are strongly associated with type 2 diabetes, cardiovascular disease, stroke, and certain cancers. Visceral fat is directly linked to hormonal belly causes, particularly elevated cortisol and insulin resistance. It’s the kind of stomach fats maximum carefully related to the classic “apple shape” that many midlife girls develop.
Subcutaneous Fat: The Pinchable Layer
Subcutaneous fats sits simply under the skin. It’s the soft, pinchable fat that you can feel when you grab your belly. While subcutaneous fat is less dangerous than visceral fat, it can still contribute to insulin resistance and inflammation whilst found in massive amounts.
Among the types of belly fat female bodies carry, subcutaneous fat is generally more responsive to diet and exercise changes. However, hormonal imbalances — particularly estrogen and cortisol dysregulation — can cause stubborn subcutaneous fat that resists standard weight-loss efforts.
Stress Belly
The stress belly is a recognizable pattern among the types of belly fat female bodies develop, characterized by fat accumulation directly in the midsection, often with a more rounded or protruding appearance. It’s driven almost entirely by elevated cortisol levels.
Women with a stress belly often describe carrying most of their weight in the stomach area while remaining relatively slim in their arms, legs, and hips. High-stress careers, anxiety disorders, and overtraining in athletes are all common contributors to this hormonal belly shape.
Hormonal Belly
A hormonal belly — often the result of estrogen imbalance, low progesterone, or perimenopause — tends to appear as a soft, lower-abdominal bulge. This is different from the hardened, upper-belly fat associated with a stress belly. Women with a hormonal belly may notice their waistband fitting tightly even when the rest of their body feels normal.
Identifying which of the types of belly fat female bodies experience you’re dealing with helps pinpoint which hormones may be out of balance and which interventions will be most effective.
How to Cure Hormonal Belly Through Lifestyle Changes

Now let’s get into the solutions. If you’ve been searching for how to cure hormonal belly fat, the good news is that targeted, strategic lifestyle changes can make a meaningful difference — even before medical intervention is needed.
Prioritize Anti-Inflammatory, Hormone-Supportive Nutrition
Diet is one of the most powerful levers you have when learning how to cure hormonal belly. The goal isn’t to slash calories dramatically — that approach can actually worsen hormonal imbalance by elevating cortisol and suppressing thyroid function. Instead, focus on foods that stabilize blood sugar, reduce inflammation, and support healthy hormone production.
Foods that aid hormonal balance:
Cruciferous vegetables (broccoli, cauliflower, Brussels sprouts) — include indole-3-carbinol, which helps wholesome estrogen metabolism
Healthy fats (avocado, olive oil, wild-caught salmon, walnuts) — essential for hormone synthesis
High-fiber foods (legumes, flaxseeds, oats) — slow blood sugar absorption and support gut health, which plays a role in estrogen regulation
Lean proteins (eggs, turkey, Greek yogurt) — stabilize blood sugar and support muscle mass
Fermented foods (kefir, sauerkraut, kimchi) — support the gut microbiome, which is directly involved in estrogen recycling
Foods to minimize include ultra-processed foods, refined sugars, refined carbohydrates, alcohol (which disrupts liver-based estrogen metabolism), and conventional non-organic dairy and meat that may contain hormone-disrupting compounds.
Strength Training: Build Muscle to Balance Hormones

When women ask how to cure hormonal belly, they often assume cardio is the answer. But strength training is actually more powerful for hormonal health in the long run. Resistance exercise improves insulin sensitivity, raises metabolism, reduces cortisol over time, and supports healthy estrogen and testosterone levels.
Aim for at least a few electricity schooling classes in keeping with the week. Compound movements — squats, deadlifts, rows, and presses — engage multiple muscle groups and produce the greatest hormonal response. Over time, building lean muscle mass increases your resting metabolic rate, making it easier to maintain a healthy weight while hormones shift.
Excessive cardio, particularly chronic high-intensity exercise, can actually worsen hormonal belly causes by keeping cortisol chronically elevated. If you’re a long-distance runner or spin class devotee who isn’t seeing results, consider replacing some of those sessions with strength work and moderate-intensity activities like walking or yoga.
Manage Stress Like It’s a Medical Prescription
Stress management is non-negotiable when learning how to cure hormonal belly driven by cortisol. This means treating stress reduction as seriously as diet and exercise.
mindfulness meditation reduces cortisol levels
Evidence-primarily based totally techniques include:
Daily mindfulness meditation — even 10 minutes per day has been shown to lower cortisol levels over time
Yoga and gentle movement — activates the parasympathetic nervous system, countering the fight-or-flight stress response
Breathwork — slow, diaphragmatic breathing signals the body to exit stress mode
Time in nature — research consistently shows that spending time outdoors reduces cortisol
Social connection — positive social relationships are among the most powerful buffers against chronic stress
Optimize Sleep for Hormonal Restoration
Sleep is while your frame restores hormonal balance. Deep sleep is associated with the release of growth hormone, which supports fat metabolism and muscle repair. During sleep, cortisol drops to its lowest levels, allowing the body to rest and recover.
To optimize sleep as part of understanding how to cure hormonal belly, establish a consistent sleep schedule, keep your bedroom cool and dark, limit screen exposure for at least an hour before bed, and avoid caffeine after noon. If you suspect sleep apnea — which is more common in women than previously believed and is associated with weight gain and insulin resistance — discuss this with your doctor.
How to Cure Hormonal Belly With Medical Support

Lifestyle changes are foundational, but sometimes hormonal belly fat requires professional medical assessment and treatment. If you’ve made consistent changes to your diet, exercise, sleep, and stress habits for several months without meaningful progress, it’s time to consult a healthcare provider who specializes in women’s hormonal health.
Get Comprehensive Hormone Testing
Standard bloodwork often misses the full hormonal picture. A thorough evaluation should include testing for estradiol, progesterone, testosterone, DHEA-S, cortisol (ideally a four-point salivary cortisol test), thyroid function (TSH, Free T3, Free T4, and thyroid antibodies), fasting insulin, and fasting glucose.
Understanding your personal hormonal baseline is essential when addressing hormonal belly causes. Without this data, treatment is guesswork.
Bioidentical Hormone Therapy
For women in perimenopause or menopause, bioidentical hormone replacement therapy (BHRT) may be an effective approach to reducing hormonally-driven belly fat. BHRT uses hormones that are chemically identical to those the body produces naturally, and when prescribed and monitored appropriately, it can help restore hormonal balance, preserve muscle mass, improve sleep, and reduce abdominal fat.
The conversation around hormone therapy has evolved significantly since the early 2000s. Current evidence suggests that for many women, particularly those under 60 who begin therapy within ten years of menopause onset, The blessings of hormone remedy outweigh the risks. Discuss this with a board-certified gynecologist or integrative medicine physician.
Medications That Support Hormonal Balance
In some cases, targeted medications may be appropriate. For women with insulin resistance, metformin or GLP-1 receptor agonists have shown significant benefits in reducing abdominal fat and improving metabolic function. For women with PCOS, specific interventions targeting androgen excess may reduce hormonal belly causes associated with that condition.
Thyroid medication for hypothyroidism, when properly dosed, can meaningfully improve metabolism and reduce belly fat in women with an underactive thyroid.
It’s important to work with a provider who takes a comprehensive, root-cause approach rather than simply treating isolated symptoms.
Gut Health and the Estrobolome
Emerging research points to the role of the gut microbiome — specifically a collection of gut bacteria called The estrobolome — in regulating estrogen levels. When gut health is compromised, the estrobolome cannot properly process estrogen, which can lead to either excess circulating estrogen or insufficient estrogen levels.
best foods to balance hormones naturally
Supporting gut health through diet, probiotics, and minimizing unnecessary antibiotic use may be an important and often-overlooked strategy in addressing hormonal belly causes at a deeper level.
Putting It All Together: A Strategic Approach
Understanding the full landscape of hormonal belly fat empowers you to stop fighting your body and start working with it. Here’s a concise motion framework:
Week 1–2: Assess and Establish Baselines
Schedule a complete hormone panel together along with your doctor
Begin a food and symptom journal to identify dietary triggers and patterns
Prioritize sleep hygiene and aim for 7–9 hours per night
Week 3–4: Build Your Hormonal Foundation
Adopt an anti inflammatory consuming sample targeted on complete foods
Begin electricity schooling to 3 instances in keeping with week
Introduce a daily stress reduction practice (meditation, breathwork, or yoga)
Month 2 and Beyond: Optimize and Adjust
Review hormone test results with your provider
Adjust dietary and supplement strategies based on your specific deficiencies
Consider working with a registered dietitian who specializes in hormonal health
Reassess body composition rather than focusing solely on the scale
The scale does not inform the total story. As you build muscle and lose visceral fat, your weight may change less dramatically than your measurements, how your clothes fit, and how you feel.
Conclusion

Hormonal belly fat is not a personal failure — it’s a physiological reality that millions of American women are navigating. The frustration of doing everything “right” and still not seeing results is real, and it deserves a real answer.
By understanding what causes belly fat in females at the hormonal level, recognizing the different types of belly fat female bodies store, identifying specific hormonal belly causes in your own life, and learning how to cure hormonal belly through both lifestyle And clinical strategies, you currently have a roadmap that is going some distance past ordinary eating regimen advice.
The path to a flatter belly and better hormonal health isn’t quick or linear — but it is absolutely achievable. Start with the fundamentals: eat whole foods, strength train, sleep deeply, manage stress, and get your hormones tested. Then build from there, with the guidance of a knowledgeable healthcare provider, and give your body the time And guide it desires to rebalance.
Your hormones can work with you — and with the right approach, they will.
This article is meant for informational functions best and does now no longer represent clinical advice. Always consult with a qualified healthcare provider before making changes to your diet, exercise, or medical treatment plan.
